Your Blood Pressure Reading Is Probably Wrong—Here's Why Doctors Keep Missing It
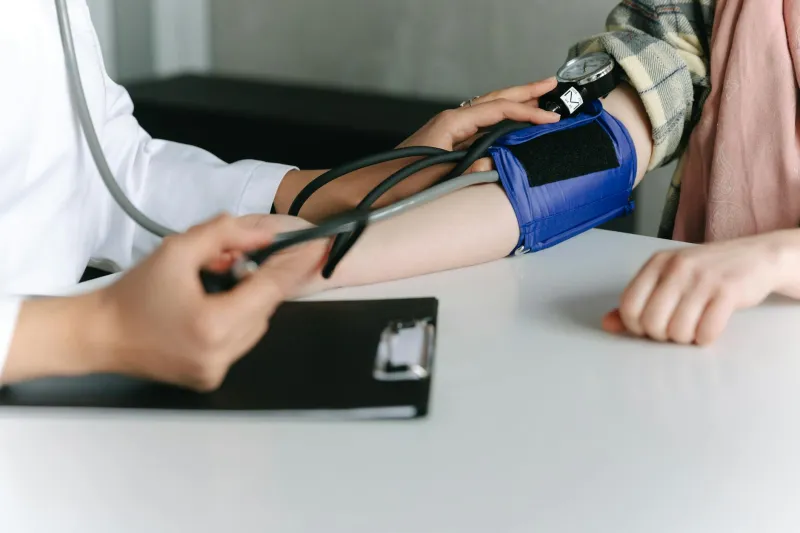
The Numbers That Shape Medical Decisions
Every year, millions of Americans walk into doctor's offices and get their blood pressure checked. Many walk out with new diagnoses, prescriptions, or stern warnings about cardiovascular health. But here's something most patients—and many healthcare providers—don't realize: the way blood pressure gets measured in most clinical settings is systematically wrong.
Cardiovascular researchers have spent decades studying proper blood pressure measurement technique. Their findings suggest that common practices in medical offices, pharmacies, and even hospitals can inflate readings by 10-40 points—enough to push someone from "normal" into "high blood pressure" territory.
The Measurement Mistakes Happening Everywhere
Walk into most medical offices, and you'll see the same routine: patient sits on an exam table, feet dangling, arm hanging at their side while the nurse wraps a cuff around it. Maybe the patient is chatting nervously about their symptoms. This scene plays out thousands of times daily across America, and nearly every element of it violates established measurement protocols.
The American Heart Association's official guidelines are specific: feet should be flat on the floor, back supported, arm at heart level, and the patient should remain silent for at least five minutes before and during the reading. The cuff should cover 80% of the arm circumference, and the bottom edge should sit one inch above the elbow crease.
 Photo: American Heart Association, via sanfernandosun.com
Photo: American Heart Association, via sanfernandosun.com
Yet a 2019 study published in the Journal of Clinical Hypertension found that healthcare providers followed proper technique less than 25% of the time. The most common errors? Wrong cuff size (used in 61% of measurements), unsupported arm (52%), and talking during the reading (48%).
Why These 'Small' Details Matter So Much
Each measurement error pushes readings higher in predictable ways. Having your feet dangle instead of resting flat on the floor can add 6-10 mmHg to your systolic pressure. An unsupported arm can add another 10 mmHg. Using a cuff that's too small for your arm can inflate readings by 2-10 mmHg. Talking during the measurement? That's another 10-15 mmHg.
Do the math: a patient with a true blood pressure of 125/80 could easily measure 155/95 in a typical clinical setting. That's the difference between "slightly elevated" and "stage 2 hypertension"—a diagnosis that could trigger medication, lifestyle restrictions, and years of follow-up care.
Dr. Michael Rakotz, who led the American Medical Association's blood pressure measurement improvement initiative, calls it "the most important vital sign we consistently measure incorrectly." The implications extend far beyond individual patients. If measurement errors are systematic, they could be inflating America's hypertension statistics and leading to overdiagnosis on a massive scale.
The Insurance and Pharmacy Problem
The measurement problems aren't limited to doctor's offices. Those blood pressure kiosks in pharmacies and grocery stores? They're often worse. A 2020 study found that 70% of public blood pressure machines hadn't been calibrated in over a year, and most lacked proper cuff sizes for different arm circumferences.
Insurance companies increasingly use these readings for health assessments and premium calculations. Some employers require blood pressure screenings for wellness programs. But if the measurements are systematically inflated, millions of Americans might be paying higher premiums or facing health restrictions based on faulty data.
What Happens When You Measure Correctly
Several medical systems have experimented with proper measurement protocols. When the Kaiser Permanente Northern California system implemented standardized blood pressure measurement across their network, they saw average readings drop by 5-7 mmHg system-wide. That wasn't because patients got healthier overnight—it was because they started measuring accurately.
 Photo: Kaiser Permanente Northern California, via nursingncal.kaiserpermanente.org
Photo: Kaiser Permanente Northern California, via nursingncal.kaiserpermanente.org
The Cleveland Clinic found similar results when they required five minutes of quiet rest before measurements and used properly sized cuffs. Hypertension diagnoses dropped by 15%, and medication adjustments were needed for thousands of patients whose previous readings had been artificially elevated.
 Photo: Cleveland Clinic, via seeklogo.com
Photo: Cleveland Clinic, via seeklogo.com
The Home Monitoring Reality
Interestingly, when patients measure their own blood pressure at home using validated devices, their readings are often significantly lower than clinic measurements—even when they're not following perfect technique. This "white coat effect" has been recognized for decades, but it's often compounded by the measurement errors that happen in clinical settings.
Many cardiologists now consider home blood pressure monitoring more reliable than office readings, precisely because patients can take multiple measurements in a relaxed environment with proper positioning.
The Simple Fix Nobody Uses
The solution isn't complicated or expensive. Proper blood pressure measurement requires about five extra minutes and attention to basic positioning. Some medical practices have designated quiet spaces specifically for blood pressure measurement. Others use automated devices that take multiple readings and calculate averages.
But healthcare economics work against accuracy. In a system where providers are pressured to see more patients in less time, spending five minutes on proper blood pressure technique feels like a luxury few can afford.
What You Can Do About It
If you're getting your blood pressure checked, you can advocate for proper measurement. Ask to sit quietly for five minutes before the reading. Make sure your feet are flat on the floor and your arm is supported at heart level. If the cuff feels too tight or too loose, ask for a different size.
Better yet, consider investing in a home blood pressure monitor validated by the American Heart Association. Take readings at the same time each day, following proper technique, and bring those numbers to your doctor. It might paint a very different picture of your cardiovascular health than those rushed office measurements suggest.